On the day of one of the deadliest natural disasters in Hawaii’s history, Blake Kekoa Ramelb watched his hometown go up in flames.
It was Aug. 8, 2023, and Maui was burning. Ramelb, born and raised in Lahaina, lived outside the burn zone, so his home was intact. But he couldn’t get into town to check on his family. He was forced to watch from afar as the fires blazed through the night, killing at least 102 people, burning down more than 2,200 structures and displacing thousands of residents.
Ramelb, a content creator and filmmaker, threw himself into community outreach and advocacy, handing out air purifiers in the burn zone and interviewing hundreds of members of his community about their loss, grief and trauma.
He rarely stopped to think about his own mental well-being. He had survivor’s guilt, he said, and was focusing his energy on those whose trauma he felt was more acute. Now, two-and-a-half years later, it’s catching up to him.
“I’m in it right now, to tell you the truth,” he said. “I didn’t deal with my own trauma or allow myself to feel the emotions that came up. … I was just so focused on everyone else that I couldn’t do that for myself.”
A paper published Wednesday by researchers from the University of Hawai‘i found that Maui residents—both directly and indirectly impacted by the wildfires—experienced high levels of psychological distress in the first year and a half after the disaster.
The study also found that more than half of the measured increase in depression and anxiety was linked to housing insecurity and job loss, illustrating how investments in social and economic infrastructure are inextricably tied to public health.
The findings have significant implications for recovery, said Ruben Juarez, the lead author and co-director of the Maui Wildfire Exposure Study, known as MauiWES.
“It allows us to focus now on solutions,” said Juarez, an economics professor at the University of Hawai‘i.
The paper is the latest in a string of research from MauiWES focused on the ongoing health burdens faced by wildfire survivors, as persistent shortages of housing and access to medical care complicate a slow recovery. Over the past two years, researchers have partnered with healthcare providers and community organizations in Hawaii to connect participants with physicians, therapists and other basic resources for their mental, physical and social well-being.
“Recovery is not just about rebuilding homes,” Juarez said. “It also means rebuilding mental health, stability and livelihoods for the entire Maui population.”
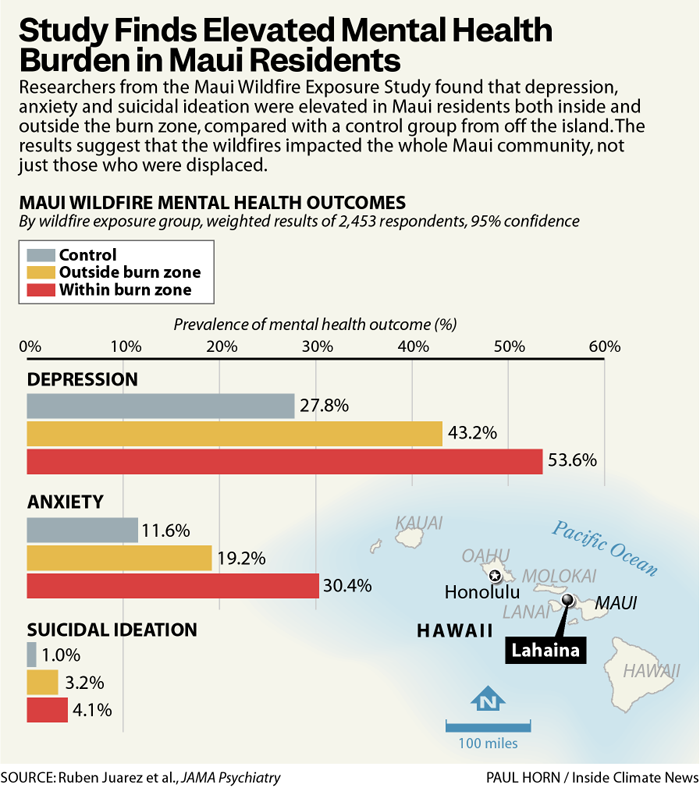
The study compares depression, anxiety and suicidal ideation among Maui residents who lived inside the burn zone during the fires, Maui residents living outside of the burn zone and residents elsewhere in the state, the latter acting as a control group. The sample included 2,453 adults.
Post-traumatic stress disorder, although prevalent in many survivors, was not included due to insufficient data from the non-Maui control population.
The results were clear: The wildfires had a broad and significant impact on residents across Maui, both inside and outside the burn zone.
After accounting for demographic differences in the populations, researchers found that symptoms of clinical depression were reported by 43 percent of Maui residents outside the burn zone and more than half of those living inside the zone, compared with 28 percent of non-Maui residents.
The clinical anxiety rate among participants in the Maui burn zone was more than twice that of the control group, and anxiety in Maui outside the burn zone was also significantly elevated.
Alika K. Maunakea, co-director of MauiWES and a co-author on the study, said researchers expected to find elevated psychological distress in those directly impacted by the fires, but the acute impact on residents outside the burn zone was somewhat surprising.
“It’s not only limited or constrained to those individuals within the burn zone, but definitely spread out to the community at large within Maui,” said Maunakea, a biomedical scientist studying epigenetics at the University of Hawai‘i’s John A. Burns School of Medicine.
Unstable housing and job loss accounted for more than half the elevated depression rate among Maui residents compared to the control group, and two-thirds of the increased anxiety, the study found.
Jeffrey I. Gold, a clinical psychologist and professor at the University of Southern California’s Keck School of Medicine, said the MauiWES team’s insight about the strong link between housing and mental health is an important finding that goes beyond the obvious reality that mental health suffers after a disaster.
“It should make other disaster researchers pay attention to not just reporting incidents of mood problems or mental health problems, but trying to contextualize it,” Gold said. “I commend them for doing that.”
Gold leads mental health outreach for the Los Angeles Fire Human Exposure and Long-Term Health Study, a multi-institution collaboration investigating environmental exposures and health outcomes in the aftermath of the deadly January 2025 wildfires in the Los Angeles area. In his own work with wildfire survivors in Altadena, he has seen how social factors like housing and insurance can exacerbate challenges to mental health.
The Maui study articulates how psychological distress among wildfire survivors goes beyond loss, also encompassing the many barriers to rebuilding, Gold explained.
“I don’t think people are thinking about that,” he said. “It’s a good discovery that’s shedding light on something other than just a person’s mental health response in isolation, in that vacuum. It’s really about how these other factors are complicating their mental health.”
Although the new study focuses on survey results from the first year and a half after the fire, MauiWES researchers and partners continue to gather data from participants and emphasize that the crisis is ongoing. They hope to continue the study for a decade and offer a blueprint for other communities recovering from wildfires.
“Consistently Reminded” of the Wildfires
Ramelb has started processing his own experience with the fires. Although his grandparents—who lived close to the burn zone—survived that day, they had to evacuate for about a month due to poor air quality, and his grandfather died soon after. Ramelb wonders if the stress and loss of routine hastened his passing.
Now, Ramelb has dreams about stories he’s heard over the past two years. When he drives through Lahaina, he is plagued by secondhand knowledge of painfully specific devastation on nearly every street.
“I almost know the entire story of everywhere I go in Lahaina,” he said. “I have all this knowledge of what happened that day and have seen so much footage or talked to so many people about it. … I’m consistently reminded of the day itself.”
Christopher Knightsbridge, a doctoral-level mental health practitioner at the Maui County Certified Community Behavioral Health Clinic, has a caseload of more than 100 patients. A co-author on the MauiWES paper, Knightsbridge works with even more survivors through the study.
“It is a crisis. We need more support.”
— Christopher Knightsbridge, a mental health practitioner
Knightsbridge said many of his patients are still in acute crisis mode, particularly those living in temporary housing. In severe cases, he has seen people self-medicating with alcohol or experiencing suicidal thoughts. But even with widespread trauma, mental healthcare is still a low priority for people who are struggling to meet basic needs, Knightsbridge said.
“Imagine you have this horrible, the worst thing that could ever happen to you,” he said. “You have to find housing, you have to find food, your kids are traumatized so you’ve got to try to be strong in front of them. … Therapy is the last thing that you’re going to think of, right?”
The clinic where Knightsbridge works is government-funded and operates on a sliding scale, also serving patients without insurance. But the clinic, like Maui’s entire healthcare sector, faces needs that far outpace its capacity. CCBHC has one psychiatrist and two full-time mental health providers, including himself, Knightsbridge said. He lives on Oahu and has to fly to Maui weekly to deliver services, he said.
It’s difficult to spend half of each week away from his own young kids, but the need on Maui is too great to deny. Though he sees some patients via telehealth, that doesn’t work for everyone, especially for his younger patients.
Wednesday’s paper focused only on adult participants, but psychological distress is prevalent across survivors of all ages, Knightsbridge said, adding that he has seen patients as young as 6 express suicidality.
“It is a crisis,” he said. “We need more support.”
In MauiWES’ sample of 200 Maui children aged 8 to 18, more than half screened positive for depression and 45 percent showed signs of PTSD, according to a 2025 report.
Knightsbridge’s own observation is that patients receiving care appear to be getting better. But many are not getting care. And two-and-a-half years after the disaster, there’s not enough help.
“People forget about us,” Knightsbridge said.
Diagnoses like depression, anxiety and PTSD also have ramifications for physical health, including chronic conditions and metabolic distress.
According to data collected through January 2025, nearly three-fourths of MauiWES’ cohort of 1,800 Maui adults had elevated or hypertensive blood pressure. More than a quarter showed reduced lung function.
As researchers screen residents’ physical and mental health, volunteer physicians meet with participants—who receive $100 for participating in the screening—to discuss their results and, at times, recommend that they seek follow-up care.
Dr. Martina Leialoha Kamaka, a physician based in Honolulu at the John A. Burns School of Medicine, is one of those volunteers. In the early months after the fires, she consistently saw patients with abnormally and dangerously high blood pressure and blood sugar.
This story is funded by readers like you.
Our nonprofit newsroom provides award-winning climate coverage free of charge and advertising. We rely on donations from readers like you to keep going. Please donate now to support our work.
Donate NowThese issues have persisted. Just a few weeks ago, Dr. Peggy Latare, another physician volunteer, saw two patients whose blood pressure constituted medical emergencies.
Kamaka and Latare said they can’t confirm whether these patterns of illness are connected to the fires, but they noted that in the aftermath of the disaster, stress prevented some patients from treating pre-existing conditions.
“People don’t worry about their meds when they’re worried about where they’re going to sleep, and their food,” Kamaka said. “We saw a lot of things get out of control.”
Looking Holistically at Health
MauiWES takes an intersectional approach to studying and addressing patient health. That’s why the team investigates interactions between mental and physical health, alongside social issues such as housing, healthcare access and economic stability.
The program’s integrative approach aligns with the Hawaiian concept of Mauli Ola, said co-director Maunakea, who is Native Hawaiian. Mauli Ola describes an understanding of health and healing that looks holistically at mental, physical, spiritual, social and environmental well-being and balance.
“In some ways, we’re returning to what we consider ‘ike kūpuna, our ancestral knowledge, to better inform how we can actually build our resilience against these disasters and even during the recovery,” he said.
Maunakea’s late great-grandmother was a kahuna lā‘au lapa‘au, a traditional healer focused on physical, mental and spiritual health and environmental stewardship. As he and the team put together MauiWES, he thought about what she would do to help her community in the aftermath of disaster.
“This is really part of her legacy,” he said. “Trying to be able to give back and help improve on the challenges we faced even before the disaster on Maui.”
Read More

After the LA Fires, Scientists Study the Toxic Hazards Left Behind
Story and photos by Nina Dietz
A recent report to the Hawaii state legislature from the University of Hawai‘i found a persistent physician shortage across the state’s four counties, with Maui experiencing the greatest shortage of primary care physicians. Its 35 percent shortfall is more than double the statewide level of need.
Hawaii struggles to retain physicians due to high housing prices and overall cost of living, while an aging population contributes to the rising need. The fires made that situation worse, both by prompting an exodus of physicians and destroying some medical facilities.
According to MauiWES data, healthcare disparities on the island follow racial and socioeconomic lines: Native Hawaiian, Pacific Islander and Latino populations are more likely to suffer from chronic diseases and less likely to have health insurance, with the Latino population experiencing the highest uninsured rate.
Job loss—one of the fuels of psychological distress—also resulted in many residents losing their health insurance, leaving chronic conditions untreated, Kamaka said.
“What we saw was healthcare that may not have been managed well before, and was certainly much worse after,” she said.
Kamaka and Latare, the physicians volunteering with MauiWES, both fly in from Honolulu for weekend programming about once a month. The need is staggering, and it is frustrating not to be able to provide longer-term care, Kamaka said, especially given the limited access to specialist doctors and mental health providers on Maui.
It makes her think about how poorly the country’s protocols for long-term patient management are set up for disasters that will only become more frequent, she said.
“We as a society aren’t prepared to help these communities deal with long-term recovery,” she said.
In Maui, Kamaka traces these disparities to the same extractive colonial history that fueled the fires. Lahaina, once nicknamed the “Venice of the Pacific” for its lush and verdant wetlands, was dried out when American and European companies began diverting its water to sugar and pineapple plantations, fueling an industry that sparked famine and backed the illegal overthrow of the Hawaiian Kingdom. The sugar industry was later replaced by a tourism industry that continued to extract Lahaina’s water.
Depleted waterways, along with rising temperatures, strong winds and loss of fire-protective native vegetation—all worsened by climate change—contributed to the dry conditions that made the 2023 fires so destructive.
As Lahaina rebuilds, many local residents are advocating for a return to traditional land management practices. That could help protect against the disasters that climate change may bring, including more severe wildfires.
“I hope, in the future, we can look back at what did work before all the global development,” Ramelb said.
Ramelb’s family has lived in Lahaina for a century, since his ancestors moved there from the Philippines to work on the plantations, he said. Hope for a rebuild that centers local priorities and resilience tethers him to the island.
“I’ve become so invested into making sure Lahaina becomes what our community wants Lahaina to be,” Ramelb said. “It has become a responsibility.”
Clarification: This story was updated March 12, 2026, to clarify Christopher Knightsbridge’s comments about the number of full-time providers at CCBHC. He said CCBHC has a psychiatrist and two full-time mental health providers.
About This Story
Perhaps you noticed: This story, like all the news we publish, is free to read. That’s because Inside Climate News is a 501c3 nonprofit organization. We do not charge a subscription fee, lock our news behind a paywall, or clutter our website with ads. We make our news on climate and the environment freely available to you and anyone who wants it.
That’s not all. We also share our news for free with scores of other media organizations around the country. Many of them can’t afford to do environmental journalism of their own. We’ve built bureaus from coast to coast to report local stories, collaborate with local newsrooms and co-publish articles so that this vital work is shared as widely as possible.
Two of us launched ICN in 2007. Six years later we earned a Pulitzer Prize for National Reporting, and now we run the oldest and largest dedicated climate newsroom in the nation. We tell the story in all its complexity. We hold polluters accountable. We expose environmental injustice. We debunk misinformation. We scrutinize solutions and inspire action.
Donations from readers like you fund every aspect of what we do. If you don’t already, will you support our ongoing work, our reporting on the biggest crisis facing our planet, and help us reach even more readers in more places?
Please take a moment to make a tax-deductible donation. Every one of them makes a difference.
Thank you,














