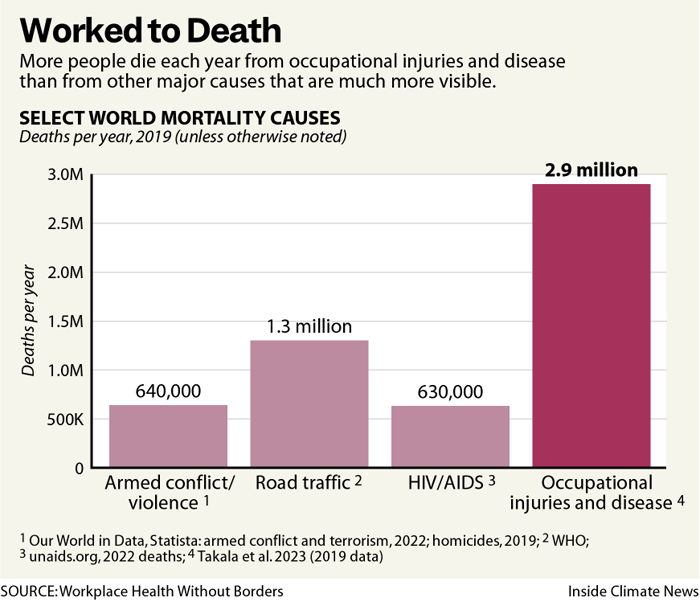
Every year, hundreds of millions of people around the world suffer from workplace injuries or illnesses, and nearly 3 million die from job-related accidents or exposures. Climate change is making many jobs even more dangerous, exposing millions of workers to excessive heat and toxic wildfire smoke each year, yet the World Health Organization has not made worker health one of its core priorities.
The well-being of the world’s nearly 4 billion workers depends on the WHO making workplace health a global priority, say senior leaders of national and global occupational health and safety organizations. They’re counting on delegates to the World Health Assembly, the WHO’s top decision-making body, to make sure the agency enshrines worker health in its strategic plans when they meet in Geneva starting May 18.
The WHO is ignoring occupational health and safety just as climate change, emerging pandemics and migration expose workers to new risks, the Global Occupational Safety and Health (GOSH) coalition said in a position paper last year.
Occupational health and safety has not gotten the attention it deserves for years, said GOSH coalition member Emanuele Cauda, a faculty member at the University of Pittsburgh focused on occupational hygiene. “We’re trying to raise awareness of the fact that leaving out occupational and safety protection for the workers is going to be a public health issue globally,” Cauda said.
Cauda and his colleagues hope to ensure that global investments in worker health match the magnitude of new and re-emerging occupational hazards.
Rising global temperatures are increasing the risk of heat-related accidents, illnesses and deaths. The rapid expansion of mining for “critical minerals” to meet renewable energy demands is exposing 100 million workers to highly hazardous chemicals and conditions. And the growing market for artificial, engineered stone in homes and construction has exposed millions in both industrialized and developing countries to a deadly dust that caused one of the worst industrial accidents in U.S. history nearly a century ago.
In 1930, thousands of men eager for work during the Great Depression began drilling a 3-mile tunnel through a West Virginia mountain as part of a hydroelectric power project. Cutting through a sandstone-rich mountain exposed workers to fine particles of the silica dust that causes an agonizing, incurable lung disease called silicosis. Even in the 1930s experts knew that ventilation, wet drilling and other precautions could prevent silicosis. Yet the workers who built Hawk’s Nest Tunnel, mostly African Americans from the South, were given no such protections. Hundreds died, as one worker recalled, “in the camps, under rocks and everyplace else.”
The tragedy triggered a congressional investigation, inspired a federal “stop silicosis” campaign, led many states to include silicosis in worker compensation laws and contributed to the passage of the Walsh-Healy Act of 1936, which prohibited companies with federal contracts from allowing dangerous working conditions. But it would take 80 years for U.S. regulators to implement federal rules restricting silica dust exposure.
The rule has done little to stop an epidemic of a rapidly advancing form of silicosis that’s emerged among workers producing artificial stone slabs for counters and other surfaces.
Now, workers in the U.S. and in several other countries are succumbing to a rapidly advancing form of silicosis, leaving young men in their thirties in need of lung transplants. Australia was the first country to ban engineered stone, but cases around the world are rising. Regulations of the $26 billion engineered stone market vary widely by country, underscoring the need for global leadership, experts say.
A Global Health Leader
Decades before the U.S. finally passed a silica dust standard, the WHO in partnership with the International Labour Organization made eliminating silicosis a priority. The U.N. agencies established the Global Programme for the Elimination of Silicosis in 1995 to prevent the incurable disease by limiting exposure in mines, construction, tunnels, sandblasting and other high-risk occupations.
Making silicosis a WHO priority for action in occupational health encouraged countries to make it a national priority, though the new wave of cases from engineered stone caught many off guard.
Yet the WHO is stepping back on past commitments to occupational health, say GOSH experts, partly due to a budgetary crisis triggered by the Trump administration’s decision to terminate its financial support last year.
President Donald Trump announced his intention to leave the WHO on the first day of his second term, citing many issues, including “unfairly onerous payments,” referring to the WHO’s mandatory assessments, which are based primarily on a country’s GDP.
The United States was the WHO’s biggest government donor, contributing around 18 percent of its overall funding, said Nick Pahl, a GOSH member and CEO of the United Kingdom’s Society of Occupational Medicine. Now, the WHO is dealing with significant budget cuts overall and even more for specific core programs, Pahl said.
“Occupational health was part of their program priorities in 2024-25, but it’s not appearing now,” Pahl said.
This story is funded by readers like you.
Our nonprofit newsroom provides award-winning climate coverage free of charge and advertising. We rely on donations from readers like you to keep going. Please donate now to support our work.
Donate NowThe WHO did not respond to multiple requests for comments about why it deprioritized occupational health. In its 2026-2027 budget, the agency said the $700 million decrease in core program funding “responds to the current and evolving global financing environment.”
Pahl urged WHO Director-General Tedros Adhanom Ghebreyesus to ensure workplace health “gets the attention it warrants,” in a recent letter on behalf of eight worker health and safety organizations.
The letter noted that illnesses, injuries and deaths caused by failing to protect workers costs the equivalent of nearly 6 percent of the world’s GDP, or up to $3 trillion annually.

The number of people who are dying at work is increasing beyond population growth, Pahl said.
“There’s not enough attention paid to occupational health in the global-health agenda,” said Marianne Levitsky, founding president and now board member of Workplace Health Without Borders, who convened the GOSH coalition. “That needs to be corrected.”
Levitsky is frustrated that occupational health is not a global health priority, given that millions die of work-related causes every year. “How many people need to die to say it’s a priority?” she said.
Shrinking Support
The loss of the WHO’s largest national donor is in some ways a final push in the WHO’s retreat on worker health, occupational health and safety experts say. They have watched the agency slowly pull back its focus on worker health for years.
At the first World Health Assembly in 1948, a binding agreement established the Joint ILO/WHO Committee on Occupational Health to meet every five years, said Thomas Gassert, a GOSH coalition core member and department associate in the Environmental and Occupational Medicine and Epidemiology program at the Harvard T.H. Chan School of Public Health. “The most effective work that the WHO has ever done on workplace health has been the result of these joint WHO/ILO committee meetings,” he said.
But the last time the joint committee on occupational health met was in 2003.
Gassert and many of his colleagues have long advocated for resuming the joint committee meetings and for preservation of the occupational health collaborating centers that help support worker health programs. Instead, they’ve watched a steady erosion of the WHO’s occupational health leadership and funding.
The WHO lost half of its 10 divisions, and what was left of occupational health was not adequately funded, Gassert said. The person who was responsible for the occupational health program retired in 2025 and was not replaced, he said.
Members of the GOSH coalition are trying to raise awareness about the need to take occupational health more seriously now because the election cycle for the next director-general has started. They want candidates to resuscitate occupational health at the WHO, revive the agency’s collaboration with the ILO and ensure that collaborating centers that work with institutions and universities to develop worker protection programs receive the funding they need to be effective.
It’s important that the people running for the next director-general reinstate occupational health as a program unit and secure the necessary funding, Gassert said. Risks are rising as climate change continues to impact workplaces, workers and their homes and families, exposing them to not only heat extremes and climate emergencies but increased air and chemical pollution, infectious diseases and many other challenges, he said.
“Climate change is an existential threat to human and planetary health,” Gassert said.
Heat has an impact on all the standard problems in workplace safety and health, he said, pointing to chemicals, radiation, biologics, mental health stress and workplace violence. The main clinical indication of heat stress is mental status change, he explained. “Then you have people falling, they get concussions, break their bones, they get killed. They work power tools inefficiently. They make mistakes. They get violent because they’re too hot.”
Gassert and many of his colleagues remain hopeful that the WHO will shift course and give occupational health the support it deserves.
To ensure the well-being of the billions of workers around the world, and their children as they enter the workplace, Gassert said, it’s imperative to boost climate resilience and emergency preparedness.
He’s confident that the next leaders at the WHO are ready to meet the challenge.
About This Story
Perhaps you noticed: This story, like all the news we publish, is free to read. That’s because Inside Climate News is a 501c3 nonprofit organization. We do not charge a subscription fee, lock our news behind a paywall, or clutter our website with ads. We make our news on climate and the environment freely available to you and anyone who wants it.
That’s not all. We also share our news for free with scores of other media organizations around the country. Many of them can’t afford to do environmental journalism of their own. We’ve built bureaus from coast to coast to report local stories, collaborate with local newsrooms and co-publish articles so that this vital work is shared as widely as possible.
Two of us launched ICN in 2007. Six years later we earned a Pulitzer Prize for National Reporting, and now we run the oldest and largest dedicated climate newsroom in the nation. We tell the story in all its complexity. We hold polluters accountable. We expose environmental injustice. We debunk misinformation. We scrutinize solutions and inspire action.
Donations from readers like you fund every aspect of what we do. If you don’t already, will you support our ongoing work, our reporting on the biggest crisis facing our planet, and help us reach even more readers in more places?
Please take a moment to make a tax-deductible donation. Every one of them makes a difference.
Thank you,













